Vitamin B-Complex Injection
This medication is compounded in Empower's PCAB-accredited 503A pharmacy and/or FDA-registered 503B outsourcing facility. Our quality process includes:
- Raw materials sourced from qualified, approved suppliers
- Finished product testing for potency, sterility, and endotoxins
- 100% visual inspection and AQL sampling - Certificate of Conformance generated for every batch
- Full batch review and release by our Quality Unit
- PCAB Accredited | FDA Registered | LegitScript Certified
Product Overview
Vitamin B-Complex Injection is a sterile compounded solution of essential B vitamins formulated for intramuscular (IM) subcutaneous (SQ) or slow intravenous (IV) use. Each 1 mL contains 100 mg vitamin B₁ (thiamine HCl), 2 mg vitamin B₂ (riboflavin-5′-phosphate sodium), 100 mg vitamin B₃ (niacinamide), 2 mg vitamin B₅ (dexpanthenol), and 2 mg vitamin B₆ (pyridoxine HCl).[1]
It is prepared in a 30 mL multi-dose vial with a preservative (2 % benzyl alcohol) for multiple withdrawals. This injection is typically prescribed to potentially prevent or treat deficiencies of these B vitamins and to support patients with conditions like malabsorption, increased metabolic demand, or recovery from illness where oral vitamin intake is insufficient.[1]
As a compounded product, it is not an FDA-approved commercially manufactured drug.
Administration: Vitamin B-Complex Injection is administered either intramuscularly, subcutaneously or by slow intravenous injection, as directed by a healthcare provider. The typical adult dosage is 0.25 mL to 2 mL per dose, depending on the severity of the deficiency or the clinical indication.[1] In practice, 1 mL (which provides the full 100 mg of B₁ and B₃, etc.) is a common dose for general supplementation in deficient states, but clinicians may start with lower volumes for mild deficiencies or in smaller patients. For instance, a patient with borderline low B-vitamin levels might receive 0.5 mL IM weekly, whereas someone with severe malabsorption could receive 1-2 mL IM two to three times per week initially. The exact dosing schedule should be individualized by the treating physician based on the patient’s needs.
Route: Intramuscular injection (into a muscle, such as the gluteus or deltoid) is the most frequent route for this therapy, as it allows the vitamins to be absorbed over time from the muscle depot. IM administration should be done with an appropriate needle to reach muscle tissue, and the site should be rotated (for example, alternate buttocks) if injections are repeated regularly to avoid soreness. Subcutaneous injection (into fat tissue) is commonly used for amounts less than 0.5 mL. Slow IV injection is an option when immediate availability of the vitamins is desired or if the patient is already receiving IV fluids. If given IV, it must be injected slowly (often over at least 5 minutes or diluted in a larger volume bag and infused).[1] This is to reduce the risk of hypotension or vein irritation; rapid IV push of concentrated B vitamins can cause dizziness or flushing. High concentrations for IV use should be diluted in normal saline or another compatible IV fluid before administration.[1] For example, if a 2 mL dose (full 200 mg thiamine, 200 mg niacinamide) is to be given IV, a nurse might mix it into 50 mL of saline and infuse over 15-30 minutes.
Frequency: The dosing frequency depends on the indication. In deficiency treatment, this injection might be given daily or every other day for a short period. For instance, hospitalized patients with severe alcohol-related malnutrition might receive 1 mL IM daily for a week. For maintenance or prophylactic use (such as in a patient with short-gut syndrome who cannot absorb oral vitamins well), a common regimen is 1 mL IM once weekly. Some protocols call for an initial loading phase (e.g. 3 times per week for 2 weeks) followed by a maintenance phase (weekly or biweekly injections). The healthcare provider will determine the regimen; patients should strictly follow the prescribed schedule.
Titration: There is generally no need for upward titration with B-complex vitamins as one might do with certain drugs, but if a patient is frail or known to react to injections, the provider may choose to start at a lower dose (for example 0.25-0.5 mL) and then increase to 1 mL as tolerated. Niacinamide does not cause the dramatic flush of niacin, so titration to mitigate flushing is usually not necessary. That said, if any adverse effect is suspected to be dose-related, the dose can be reduced.
Missed Dose: If a patient misses a scheduled injection, they should contact their healthcare provider for advice. In general, a missed dose can be administered as soon as remembered, unless it is almost time for the next dose. In that case, the patient should skip the missed one and continue on the regular schedule; do not double up doses.[11] Because these vitamins are not long-term cumulative drugs (they don’t maintain stable plasma levels like a blood pressure medication would), missing one dose is usually not critical. The patient should simply get the next injection at the earliest convenient time. For example, if a weekly injection on Monday was missed, it could be given on Tuesday and then resume the normal schedule. Adherence to the regimen is encouraged to effectively replete or maintain vitamin levels, but occasional timing adjustments are acceptable.
Administration Precautions: Before each administration, the vial should be inspected visually for any particulate matter or discoloration. If the solution has precipitated (which can happen if it was frozen or refrigerated improperly), do not inject unless warming the vial to body temperature has fully dissolved the precipitates.[1] Use a new sterile needle and syringe for each withdrawal (multi-dose vial technique), and swab the rubber stopper with alcohol. Intramuscular injections should be given deep to minimize irritation. After injection, applying a gentle massage to the site may help distribute the fluid and reduce soreness. Patients should remain seated for a few minutes after an IM or IV dose, just to ensure they do not experience dizziness. In clinic settings, emergency measures (like epinephrine and antihistamines) should be readily available in the rare event of an allergic reaction.
Overdosage: Acute overdose with this injectable B-complex is unlikely to cause severe toxicity, as excess water-soluble vitamins are largely excreted in urine.[4] In case of accidental large overdose (e.g., someone receives far more frequent injections than prescribed), monitoring for symptoms like flushing, tingling in extremities, or liver enzyme elevations would be prudent. Treatment of such an overdose would be mainly supportive, since there is no specific antagonist for B vitamin excess; fortunately, serious consequences are rare.
In summary, the dosage and administration of Vitamin B-Complex Injection are flexible and should be tailored by the healthcare provider. The key is to use the lowest effective volume and frequency to correct the deficiency or meet the metabolic need, and to adjust as the patient’s condition improves. Patients should always follow professional instructions on how to administer (if self-injecting) or when to return for injections, and keep all scheduled appointments to ensure optimal therapy outcomes.
B-complex vitamins serve as coenzymes or precursors in numerous biochemical reactions, and together they work synergistically to support metabolism, neurological function, and cellular energy production.[3]
Thiamine (vitamin B₁) is required for carbohydrate metabolism; in its active form (thiamine diphosphate), it is an essential cofactor for enzymes in glucose and amino acid catabolism, helping convert nutrients into ATP and supporting normal neuronal function.[3]
Riboflavin (vitamin B₂) is a component of coenzymes FMN and FAD, which drive oxidative energy production and cellular respiration; B₂ is crucial for the metabolism of fats, drugs, and steroids and for the activation of other vitamins (it helps convert vitamin B₆ to its active form and aids the conversion of tryptophan to niacin).[4]
Niacinamide (vitamin B₃) forms the coenzymes NAD⁺ and NADP⁺, which are involved in hundreds of oxidation-reduction reactions in cells. These reactions are central to ATP generation, DNA repair, and cell signaling, so adequate B₃ supports energy levels and normal cell function.[5]
Pantothenic acid (vitamin B₅, provided as dexpanthenol) is a building block of coenzyme A, a critical coenzyme in the Krebs cycle and fatty acid oxidation; through CoA, vitamin B₅ participates in the synthesis of neurotransmitters, steroid hormones, and other key cellular components.[5]
Pyridoxine (vitamin B₆) is converted to pyridoxal-5′-phosphate, a coenzyme for over 100 enzymes in amino acid metabolism. B₆ is needed for the production of neurotransmitters such as GABA, serotonin, and dopamine, and for glycogen breakdown and hemoglobin synthesis.[5]
By simultaneously providing all these B vitamins, the injection ensures that the body has all necessary co-factors in adequate supply; this prevents metabolic bottlenecks that might occur if one B vitamin is lacking.
In essence, each component supports different steps of metabolic pathways, for example, energy generation from carbohydrates and fats requires B₁, B₂, B₃, and B₅ in sequence; thereby the combined administration helps optimize overall metabolism and neurological health.[3]
Patients with deficiencies often experience fatigue, cognitive or nerve impairments, and slow recovery; correcting those deficiencies with the B-Complex Injection can restore normal enzymatic function and improve cellular energy production, which supports vitality and organ function in those individuals.
Vitamin B-Complex Injection should not be used in patients with known hypersensitivity to any of its ingredients. This includes allergy to thiamine or any other B vitamin in the formulation, or to excipients like benzyl alcohol.[1]
Because the vial contains benzyl alcohol as a preservative, it is contraindicated in neonates and infants; benzyl alcohol has been associated with serious adverse events (the “gasping syndrome”) in newborns and must be avoided in this population.[6]
Patients with a history of severe allergic reactions to similar injectable vitamins should not receive this product, or should undergo desensitization under close medical supervision if the therapy is deemed essential.
High-dose niacin therapy is normally contraindicated in individuals with active peptic ulcer disease or active liver disease; similarly, while the niacinamide in this compounded B-Complex is in a moderate dose, caution is advised in patients with untreated peptic ulcers or significant hepatic impairment, as even moderate niacin supplementation could aggravate these conditions (e.g. by increasing stomach acidity or liver enzyme elevations).[7]
Use is also contraindicated in patients with arterial bleeding.[7] Niacin can cause vasodilation, so it should be avoided in those with serious hypotension; indeed, people with very low blood pressure or those prone to orthostatic hypotension should not use niacinamide injections without careful monitoring.[8]
Similarly, patients with gout or hyperuricemia should avoid high niacin intake, as niacin (even in nicotinamide form) can raise uric acid levels and potentially trigger gout flares.[8]
Although not an absolute contraindication, patients with coronary artery disease or unstable angina should only use B-Complex injections containing niacinamide under physician supervision, since high-dose niacin supplements have been linked to arrhythmias in such patients.[8]
Each individual B vitamin is water-soluble and generally very safe at physiologic doses, but the combination product should only be used when clearly needed.
In summary, this compounded injection is contraindicated in anyone with allergies to its components, in neonates, and in patients in whom even moderate doses of B₃/B₆ might pose unacceptable risks (e.g. active ulcer, serious liver disease, hypotension, or gout).
Because this formulation provides multiple B vitamins at significant doses, it is important to consider how each component might interact with medications or other supplements the patient is taking.
Pyridoxine (B₆) in high doses is known to interact with certain drugs: it can reduce the therapeutic efficacy of levodopa by increasing peripheral conversion of levodopa to dopamine (vitamin B₆ speeds up decarboxylation). For this reason, patients with Parkinson’s disease on levodopa therapy should avoid high B₆ intake unless they are also taking carbidopa (which prevents this interaction). Doses of pyridoxine as low as 5-10 mg can antagonize levodopa’s effect if carbidopa is not present, so caution is warranted and any supplemental B₆ beyond the nutritional dose should be under medical guidance.
Vitamin B₆ can also decrease serum levels of certain anticonvulsant medications; co-administration of pyridoxine has been shown to reduce the blood levels of phenobarbital and phenytoin, possibly diminishing their anticonvulsant efficacy. Patients on those medications should only receive B-Complex injections with close monitoring (and dosage adjustments of the anticonvulsant if needed).
On the other hand, several drugs can deplete pyridoxine or heighten its requirement; for example, isoniazid, cycloserine, penicillamine, and hydralazine each form complexes with B₆ or otherwise interfere with B₆ metabolism, potentially leading to deficiency and peripheral neuropathy. Such patients often are prescribed supplemental B₆; the B-Complex Injection can help mitigate drug-induced B₆ deficiency, but the clinician should be mindful to coordinate its use so that adequate B₆ is maintained without causing excessive levels.
Niacinamide (B₃), like niacin, has several notable interactions. Niacin/niacinamide may potentiate the effects of antihypertensive medications by causing additional vasodilation; if a patient is on blood pressure-lowering drugs (such as beta blockers, alpha-1 blockers, or vasodilators), niacinamide injections could lead to an additive drop in blood pressure. Careful monitoring of blood pressure is recommended when initiating therapy in hypertensive patients, and those with baseline low blood pressure should use B₃-containing injections cautiously.
Niacin can also have an antagonistic effect on gout medications: it elevates uric acid levels, which may counteract drugs like allopurinol or pegloticase that are meant to lower uric acid. Patients being treated for gout should therefore be monitored for changes in uric acid if receiving high-dose B₃; any gout flare-ups might necessitate re-evaluation of niacinamide therapy.
Additionally, niacin has been noted to increase fasting blood glucose by inducing insulin resistance in some cases; large doses might diminish the effectiveness of antidiabetic medications (like insulin, metformin, or sulfonylureas). Although the 100 mg of niacinamide in this injection is relatively modest compared to gram doses used to treat cholesterol, diabetic patients should still have their blood sugar observed, as even moderate niacinamide supplementation could necessitate small adjustments in diabetes medications.
Conversely, isoniazid and pyrazinamide (tuberculosis drugs) are structural analogs of niacin that can interfere with niacin metabolism, potentially precipitating pellagra in rare cases; such patients may require niacin supplementation, which this injection could provide.[5]
Thiamine (B₁) has no known major drug-drug interactions in terms of altering other medications’ efficacy. However, it’s worth noting that certain diuretics (e.g. furosemide) can increase urinary excretion of thiamine and thereby lower B₁ levels over time. Patients on long-term loop diuretics might benefit from B₁ supplementation, and the B-Complex Injection can help replete thiamine in those individuals.
Chemotherapy with drugs like 5-fluorouracil has also been associated with acute thiamine deficiency by disrupting thiamine activation, so oncology patients receiving such therapy might receive parenteral thiamine supplementation as part of this B-Complex if needed. These are more considerations of medications affecting vitamin status (rather than the vitamin affecting the medication), but they illustrate the clinical judgment required when co-administering this injection with certain treatments.
Riboflavin (B₂) and pantothenic acid (B₅) have fewer documented interactions. One moderate interaction to note is that oral B-complex vitamins, including riboflavin, can interfere with the absorption of tetracycline antibiotics if taken simultaneously. This is not an issue with an injection (since IM/IV bypasses the gut), but if a patient is also taking oral supplements, they should separate them from tetracycline dosing.
High doses of pantothenic acid have been reported to compete with biotin uptake in the intestines (because they share a transport mechanism); again, this is relevant mainly for oral supplementation, but it suggests caution in patients taking separate high-dose biotin supplements.[5]
Finally, combining this B-Complex Injection with other supplements containing the same vitamins (such as multivitamins or energy drinks) should be done carefully. While toxicity is rare, excessive intake of certain B vitamins (particularly B₃ or B₆) from multiple sources could increase the risk of side effects (like niacin flush or peripheral neuropathy). Patients should inform their healthcare provider of all supplements they use.
In summary, the key interactions to consider are pyridoxine’s reduction of levodopa and anticonvulsant efficacy, niacinamide’s additive effects on blood pressure, blood sugar, and gout management, and the potential need for B-vitamin repletion in patients on certain medications (diuretics, isoniazid, etc.). Close monitoring and consultation with a pharmacist or provider is advised to manage these interactions and adjust therapy as needed.
At recommended dosages, Vitamin B-Complex Injection is well tolerated by most patients, but as with any parenteral therapy, side effects can occur. Injection-site reactions are among the most commonly reported side effects: patients may experience pain, stinging, or mild burning at the IM injection site.[1] This discomfort is usually transient and can be minimized by using proper technique and allowing the solution to come to room temperature before injection. Some individuals develop a small area of redness or swelling at the injection site after IM administration; this local reaction typically resolves on its own within a day or two.
If the injection is given IV (slowly), there may be a brief sensation of warmth or a mild flushing during the infusion, owing to the niacinamide component; however, unlike nicotinic acid, niacinamide does not usually cause the intense flushing reaction (redness/itching) of the skin. In fact, the chemical form in this product was chosen to avoid that side effect; skin flushing is far less common with nicotinamide than with niacin (nicotinic acid).[9]
Because B vitamins are water-soluble, excess amounts are excreted in urine, which can lead to a noticeable change in urine color. It is normal for urine to turn a bright yellow-orange color after B-complex injection; this is due to riboflavin and its metabolites, and it is a harmless effect. Patients should be counseled that neon yellow urine is expected; it simply indicates the body is eliminating surplus riboflavin and does not signify any problem.[4]
Some individuals might experience mild diarrhea or gastrointestinal upset after parenteral B-vitamin administration.[1] Niacinamide in high doses can sometimes cause nausea, heartburn, or a sensation of warmth; in the 100 mg dose present here, serious GI effects are uncommon, but mild nausea or stomach discomfort could occur in sensitive patients.[9] Transient itching or rash has been noted in some cases, possibly indicating a mild sensitivity reaction.[1] If a rash or generalized itching develops, the injection should be halted and the patient evaluated, as it could be a prodrome of a more serious reaction.
Serious adverse effects are rare but have been reported, particularly with IV administration of thiamine. Anaphylactic reactions to thiamine are exceedingly uncommon (estimated incidence well below 1 %), but they have been documented. Parenteral thiamine can in rare instances trigger an acute allergic response characterized by hypotension, breathlessness, itching, and swelling; for this reason, some clinicians recommend an intradermal test dose in individuals who may be at risk of thiamine allergy.[1]
If during injection a patient experiences chest pain, difficulty breathing, hives, or swelling of the face or throat, it could indicate anaphylactic shock; this is a medical emergency requiring immediate intervention (epinephrine, etc.). Fortunately, such reactions are extremely infrequent; a recent safety analysis found no anaphylaxis in hundreds of patients receiving high-dose IV thiamine, suggesting the risk is very low in practice.[5] Nevertheless, any signs of hypersensitivity (such as a diffuse rash, wheezing, or feeling of throat tightness) warrant stopping the injection and seeking prompt medical care.[1]
Other rare side effects noted (mostly in older literature or high-dose use) include: polycythemia vera and peripheral vascular thrombosis in patients receiving repeated injections (though these associations are not well understood, they were listed in prior product literature as possible adverse events).[1] These are exceedingly uncommon and possibly coincidental findings.
Vitamin B₆ (pyridoxine), when chronically taken in gram quantities, is known to cause a sensory neuropathy, numbness and tingling in the extremities, but the amount of B₆ in this formula (2 mg per mL) is far below such neurotoxic levels.[5] There is essentially no risk of B₆-induced neuropathy at the doses used here, especially given the limited duration most patients use injectable therapy.
Similarly, although hepatic dysfunction can occur with large niacin doses (1-3 grams daily over months) causing elevated liver enzymes or jaundice, niacinamide at 100 mg is very unlikely to have any adverse effect on the liver. To put it in context, nicotinamide has shown signs of liver toxicity only at doses around 3,000 mg per day or higher; many times the total amount a patient would receive weekly from this injection.[9]
Overall, the safety profile of Vitamin B-Complex Injection is favorable. The most common patient complaints are minor: soreness at injection site, a transient headache, or mild diarrhea; and these tend to resolve quickly. Patients should be advised about the urine discoloration (to avoid alarm) and counseled to report any persistent side effects. If side effects like stomach upset or flushing are bothersome, the dosing schedule might be adjusted (e.g. smaller doses given more frequently).
In clinical use, significant side effects are uncommon, and the vast majority of patients tolerate the therapy without problems. All serious or unexpected adverse reactions (especially allergic responses) should be reported and the therapy re-evaluated. Ensuring proper administration technique (IM deep into muscle, or IV slowly diluted) also helps minimize adverse effects like injection pain or vein irritation.
Pregnant and breastfeeding individuals have increased requirements for many B vitamins, and indeed these vitamins are routinely included in prenatal supplements. All the components of Vitamin B-Complex Injection are essential nutrients for normal fetal development and maternal health. For example, the thiamine requirement rises during pregnancy to about 1.4 mg/day (vs. 1.1 mg in nonpregnant women) and riboflavin likewise increases to 1.4 mg/day.[4] Deficiency of B vitamins in pregnancy can lead to serious complications; severe thiamine deficiency, while rare, can cause Wernicke’s encephalopathy in hyperemesis gravidarum, and inadequate B₆ is associated with anemia and neurologic issues in the newborn. Therefore, maintaining sufficient levels is important. However, because this product provides doses far above the daily nutritional requirements (for instance 100 mg of B₁ vs an RDA of ~1.4 mg), its use in pregnancy must be carefully considered.
Thiamine (B₁) is generally recognized as safe in pregnancy and is in fact critical to prevent deficiency in pregnant patients with prolonged vomiting. Thiamine has not been associated with fetal harm; pregnant women often receive IV thiamine if needed (e.g., for hyperemesis) without issue. Pyridoxine (B₆) is notably used during pregnancy to treat nausea and vomiting; the combination of vitamin B₆ and doxylamine is an FDA-approved remedy for morning sickness. Pyridoxine is categorized as pregnancy category A, meaning controlled studies have shown no risk to the fetus. This indicates that vitamin B₆ at therapeutic doses is very safe in pregnancy. In fact, adequate B₆ can improve pregnancy outcomes, and deficiency is common if supplementation is not given. Riboflavin (B₂) and pantothenic acid (B₅) have no known teratogenic effects; they are routine constituents of prenatal vitamins and are considered safe when used at recommended doses. No specific pregnancy classification exists for riboflavin or pantothenate in the U.S. (the FDA has exempted many vitamins from formal categorization), but they are regarded as safe as part of a normal diet and necessary for fetal growth.
Niacinamide (B₃) in high pharmacological doses has less pregnancy data. Niacin (nicotinic acid) has been classified as pregnancy category C; meaning that animal studies have shown some adverse effect or there are no well-controlled studies in humans, but potential benefits may warrant use despite potential risks.[9] High-dose niacin (used to treat cholesterol) lacks human safety data in pregnancy and could theoretically affect the fetus (for example, by causing hypotension or altering lipid metabolism). However, niacinamide at physiological doses (like those in prenatal vitamins or moderate supplements) is not known to be harmful. The 100 mg niacinamide in this injection is higher than the RDA (18 mg NE in pregnancy) but still far below levels used in lipid therapy. If needed for a clear medical indication (such as treating pellagra in a pregnant patient), niacinamide can be used with caution, but unnecessary high-dose B₃ supplementation is avoided in pregnancy.
Given these considerations, Vitamin B-Complex Injection should be used during pregnancy only if clearly indicated. If a pregnant patient has a documented deficiency of one or more B vitamins or a condition like hyperemesis that prevents oral intake, the benefits of correcting the deficiency (preventing serious maternal and fetal complications) outweigh any minimal risk from the injection. Each ingredient on its own is either Category A (B₆) or essential with no evidence of harm at normal levels (B₁, B₂, B₅) or Category C in very high doses (niacin). Clinicians will typically try standard prenatal vitamins or oral supplementation first, resorting to IM/IV B-complex therapy if those are inadequate or not feasible. When used, monitoring of maternal vital signs and general condition can provide reassurance that no adverse reactions (like excessive hypotension from niacinamide) are occurring. No congenital abnormalities have been linked to these vitamins at the doses provided; indeed, severe deficiencies of B vitamins are a known danger to pregnancy, whereas supplementing them is generally beneficial.
For breastfeeding, the water-soluble vitamins readily pass into breast milk. Lactating women have higher daily needs for B vitamins (for instance, riboflavin 1.6 mg/day, niacin ~17 mg NE/day), because some of the maternal intake is secreted in milk to nourish the infant.[4] Normal levels of B vitamins in breast milk are desirable, as they support the infant’s developing metabolism. Use of Vitamin B-Complex Injection in a breastfeeding mother will sharply raise her plasma levels of these vitamins, leading to enriched levels in her breast milk. This is not inherently dangerous; the infant will simply receive more B vitamins, and excess will be excreted in the infant’s urine as well. However, high-dose niacin (as a medication for cholesterol) is generally not recommended during breastfeeding, because significant amounts could enter milk and cause unwanted effects in the nursing infant (flushing, for example).[9]
The doses in this compounded injection are much lower than those therapeutic megadoses, but still higher than typical dietary intake. One study found that lactating women taking 2-60 mg of niacin daily had milk niacin concentrations of 1.17-2.75 μg/mL. With 100 mg nicotinamide administered, levels in milk would likely rise further; while there is no evidence of harm at that level, caution is advised. The recommended daily intake of niacin for lactation is ~17-20 mg, which is easily met by a normal diet.[9] Therefore, unless the mother has a clear deficiency, routine use of the B-Complex Injection during breastfeeding may be unnecessary. If the injection is needed (e.g., to replete B₁ or B₆ in a deficient mother), it can be used, but the infant should be observed for any unusual symptoms (though none would be expected from B vitamins, apart from perhaps looser stools if anything).
In summary, each vitamin in this injection is either Category A (pyridoxine) or exempt but considered safe at normal intake (thiamine, riboflavin, pantothenic), except niacin which is Category C at high doses but likely safe at modest doses. The injection should be given in pregnancy only if indicated, and under healthcare supervision. It is not a routine prenatal supplementation method but rather a therapeutic intervention for specific needs. When used, it can correct deficiencies that might otherwise jeopardize pregnancy outcomes, thus its judicious use can be very beneficial. Pregnant or breastfeeding patients should discuss with their obstetric provider before starting this injection, and ensure all healthcare team members are aware, so that vitamin levels and any pregnancy-related effects can be monitored appropriately.
Proper storage of the Vitamin B-Complex multi-dose vial is essential to maintain its stability and potency. Refrigeration is required: store the vial at 2°-8°C (36°-46°F). The product should be kept in a refrigerator when not in use, and not left at room temperature for prolonged periods, except for drawing up a dose. Do not freeze the vial. Freezing can cause the vitamins (especially riboflavin and perhaps dexpanthenol) to precipitate or the solution to phase-separate; if the medication accidentally freezes during shipping or storage, it may form crystals or cloudiness.[6] If that occurs, it can sometimes be salvaged by allowing it to warm to room temperature; if the precipitate re-dissolves completely with gentle warming and shaking, the solution may be usable. However, if any particulate matter remains undissolved or the solution remains cloudy, the vial should be discarded for safety.[1] Always inspect the solution in good light before withdrawing a dose: it should appear clear and free of particles or haze.
Protect from light: The vial should be stored in its original carton or another light-resistant container until use. Riboflavin (vitamin B₂) is light-sensitive and can degrade with exposure to sunlight or strong UV light, which may reduce the vitamin content and cause the solution to darken. The manufacturer explicitly advises keeping the vial in the carton to shield it from light.[1] If the solution is drawn into a syringe for injection, it should be administered promptly for the same reason (avoid leaving the filled syringe exposed to light for long).
It is normal for the solution to darken slightly over time under refrigeration, particularly due to the riboflavin content. A slight yellow-orange coloration or darkening does not indicate loss of efficacy; the product information notes that refrigeration can cause a color change (darker yellow) which does not affect safety or effectiveness.[1] However, any pronounced color change (for example, turning brown) or development of a precipitate should be treated with caution. If in doubt, one should consult the pharmacy or manufacturer for guidance or replace the vial with a fresh supply.
Keep the vial tightly sealed. After each use, ensure the rubber stopper is clean and the cap is on, then return the vial to refrigerated storage. Since this is a multi-dose vial with a preservative, it can be used for multiple doses in the same patient. Nonetheless, it should be used within a certain timeframe as recommended by the pharmacy (often 28 days after first puncture, per general guidelines for multi-dose vials, unless otherwise specified). Marking the date of first use on the label can be helpful. Do not use the vial beyond its labeled expiration date. Expired vitamin solutions may have reduced potency and an increased chance of contamination or chemical breakdown.
The vial should be kept out of reach of children, as with any medication. In a clinical setting, it will be stored in the medication refrigerator. In a home setting, patients should have a designated spot in their refrigerator to store it safely (ideally in a container to avoid contact with food items and with the original box around it). It’s recommended not to freeze (as mentioned) and also to avoid excessive heat; so do not place it near the freezer compartment where freezing could occur, and don’t leave it at room temperature or in a hot car. If the patient needs to transport the medication (e.g., traveling), it should be carried in a cooler bag with ice packs to maintain the cold chain.
By adhering to these storage instructions, keep cold, protect from light, do not freeze, check for clarity, the integrity of the Vitamin B-Complex Injection can be ensured for the duration of its use. Improper storage could lead to vitamin degradation (losing potency) or increased risk of injection site reactions (if contaminants or precipitates form), so patients and providers should take the storage guidelines seriously. When stored correctly, this compounded injection remains stable and effective until the stated expiration.
- Mylan Institutional LLC. (2021). Vitamin B-Complex 100 Injection [Prescribing information]. Revised 09/2021. (Contains description of formulation, indications, dosing, and storage recommendations). (https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=282ccec8-9bcd-4571-9b91-bbb96ef2620d
- U.S. Food & Drug Administration. (2018). Compounded drugs are not FDA-approved. In Human Drug Compounding: Laws and Policies. FDA.gov. (Explains that compounded medications under Section 503A are exempt from FDA pre-market approval requirements, meaning their safety and efficacy are not evaluated by FDA prior to use). (https://www.fda.gov/drugs/human-drug-compounding/human-drug-compounding-laws
- Kennedy, D. O. (2016). B Vitamins and the Brain: Mechanisms, Dose and Efficacy - A Review. Nutrients, 8(2), 68. https://doi.org/10.3390/nu8020068 (Comprehensive review detailing the inter-related roles of B-complex vitamins in cellular metabolism, energy production, and neurological function). (https://doi.org/10.3390/nu8020068
- Harvard T.H. Chan School of Public Health. (n.d.). Riboflavin - Vitamin B2 (Fact Sheet). The Nutrition Source. Retrieved May 3, 2025, from https://www.hsph.harvard.edu (Notes that riboflavin is a key coenzyme in energy metabolism; excess is excreted in urine, often causing bright yellow coloration, and no upper toxicity level has been observed). (https://nutritionsource.hsph.harvard.edu/riboflavin-vitamin-b2/
- Abosamak, N. R., & Gupta, V. (2023). Vitamin B6 (Pyridoxine). In StatPearls [Internet]. StatPearls Publishing. (Updated August 17, 2023). (Provides pharmacological details on pyridoxine, including its role as a coenzyme in neurotransmitter synthesis and interactions such as the antagonism of levodopa and reduction of phenytoin levels). (https://www.statpearls.com/point-of-care/640
- McGuff Medical. (2023). Vitamin B Complex 100 Injection (with Dexpanthenol) - Product Information. McGuff.com. (Product listing for a similar compounded B-complex injection; includes warnings that parenteral thiamine may cause anaphylaxis and that the benzyl alcohol preservative is contraindicated in neonates due to risk of serious reactions). (https://www.mcguff.com/vitamin-b-complex-100-injection-with-dexpanthenol-multiple-dose-vial-30-ml
- Djadjo, S., & Bajaj, T. (2023). Niacin (Vitamin B3). In StatPearls [Internet]. StatPearls Publishing. (Updated March 20, 2023). (Outlines contraindications for niacin therapy, including active peptic ulcer disease, active liver disease with elevated enzymes, hypersensitivity to niacin, and arterial bleeding, as well as monitoring recommendations for blood pressure, glucose, uric acid, etc., due to niacin’s systemic effects). (https://www.statpearls.com/point-of-care/38460
- Mount Sinai Health Library. (n.d.). Vitamin B3 (Niacin). Retrieved May 3, 2025, from https://www.mountsinai.org/health-library/supplement/vitamin-b3-niacin (Cautions that people with low blood pressure or a history of gout should not take niacin/niacinamide due to risk of hypotension and hyperuricemia; also notes need for medical supervision in coronary artery disease). (https://www.mountsinai.org/health-library/nutrition/niacin
- Drugs.com. (2023). Niacin - Pregnancy and Breastfeeding Warnings. Retrieved May 1, 2025, from Drugs.com database. (States that niacin should be used in pregnancy only if the benefit outweighs the risk; classified as FDA Pregnancy Category C. Notes that high-dose niacin passes into breast milk and that lipid-altering doses could pose risks to nursing infants, recommending caution or avoidance of such doses during breastfeeding). (https://www.drugs.com/pregnancy/niacin.html
- Drugs.com. (2024). Pyridoxine (Vitamin B6) - Pregnancy and Breastfeeding Warnings. Retrieved May 1, 2025. (Documents that pyridoxine is FDA Pregnancy Category A with increased requirements in pregnancy and is commonly used to treat morning sickness. Indicates that no adverse fetal effects have been observed at normal doses and that pyridoxine is considered safe and often beneficial in pregnancy. Also notes it is excreted in breast milk but is safe at nutritional levels). (https://www.drugs.com/pregnancy/pyridoxine.html
- National Institutes of Health, Office of Dietary Supplements. (2022). Niacin: Fact Sheet for Health Professionals. Retrieved from https://ods.od.nih.gov (Provides insight into niacin’s safety profile: nicotinic acid commonly causes flushing at doses ≥30 mg; high pharmacologic doses (1-3 g/day) can cause hypotension, insulin resistance, and hepatotoxicity. Nicotinamide (niacinamide) does not cause flushing and has fewer side effects, with nausea and liver toxicity reported only at very high intakes ~3 g/day). (https://ods.od.nih.gov/factsheets/Niacin-HealthProfessional/
- Cleveland Clinic. (2025). General Medication Guidelines - Missed Dose Instructions. In Patient Education - Vitamins. ClevelandClinic.org. (Advises that if a dose is missed, take it as soon as possible unless it’s almost time for the next dose, in which case skip the missed dose. Emphasizes not to double doses. This general rule applies to maintaining consistent supplementation schedules for vitamins). (https://my.clevelandclinic.org/health/drugs/23803-vitamin-b-complex-tablets-or-capsules
What is Vitamin B-Complex Injection and why do I need it?
Vitamin B-Complex Injection is a combination of five essential B vitamins (B₁, B₂, B₃, B₅, B₆) in a sterile solution. It’s designed to rapidly replenish these vitamins in your body when you cannot get enough from oral supplements or diet. Your doctor may prescribe it if you have a documented B-vitamin deficiency or a condition like malabsorption, severe gastrointestinal issues, or after certain surgeries where your body’s demand for B vitamins is higher. Unlike standard oral multivitamins, this injection delivers the nutrients directly into muscle or bloodstream, ensuring full absorption. It is especially useful “where oral intake is insufficient or absorption is compromised,” as noted in the product literature.[1] This is a prescription compounded medication, meaning it’s made by a specialized pharmacy for you; it is not a mass-produced, commercial vitamin shot. The goal of therapy is to restore normal levels of these vitamins in your system, which may improve symptoms like fatigue, nerve pain or brain fog if they were caused by deficiencies. In short, it’s a targeted nutritional intervention to support your metabolism and health under your doctor’s guidance.
Is this injection approved by the FDA?
All the vitamins in this injection are naturally present in foods and are essential to the human body. The most common side effect is some soreness at the injection site, and you might notice your urine turning bright yellow (that’s just the excess vitamins, particularly riboflavin, being excreted).[4] Serious reactions are extremely rare; however, anytime you receive an injection there’s a slight risk of allergic reaction. Your healthcare provider will monitor you, especially with the first dose. Regarding FDA approval: because this is a compounded product, it is not directly FDA-approved.[2] The FDA approves manufactured drugs that undergo extensive clinical trials. Compounded medications are exempt from that process; they are prepared by pharmacists according to a physician’s specifications when a suitable approved product isn’t available. That said, the components, the vitamins themselves, are well studied, and compounders must adhere to strict quality standards. Essentially, the FDA has not formally evaluated this exact mixture for safety/efficacy, but each ingredient’s effects are well-known. The pharmacy preparing it follows regulations to ensure the product’s quality. You should use this injection only under medical supervision and exactly as prescribed. If you have concerns, discuss them with your doctor; they can explain why the benefits for your particular case outweigh any risks. Rest assured that your provider has recommended this therapy because they believe it’s the best way to address your nutritional needs.
How and where do I administer the injection? Can I do it myself?
Vitamin B-Complex Injection can be given either intramuscularly (IM), usually into a large muscle like the upper outer buttock (gluteal muscle) or thigh, subcutaneously (SQ) or sometimes intravenously (IV) as a slow injection in a clinical setting.[1] Most often for at-home therapy, it will be IM injections. If you are going to self-administer at home, your healthcare provider or nurse will teach you proper technique. This includes cleaning the injection site with alcohol, using a sterile syringe and needle, and injecting into the muscle at a 90-degree angle. Common sites for self-injection are the thigh (vastus lateralis muscle) or the hip area. The deltoid (upper arm) is also an IM site but can be harder to reach on your own. Many patients or their family members are capable of giving IM injections after appropriate training. If you’re uncomfortable with self-injection, you can arrange to have a nurse or health professional administer it at an office or clinic.
For IV use, typically that’s done in a medical facility (hospital or infusion center). The injection would be given slowly into a vein, or added to an IV drip. IV administration might be chosen if you are already on IV fluids or need a very rapid correction of vitamin levels. But for most purposes (like weekly maintenance injections), IM is the preferred route at home because it’s simpler (the vitamins absorb quickly from muscle into the bloodstream over a few hours).
When preparing your IM injection, draw up the prescribed amount (for example, 1 mL) into the syringe. It’s normal for the solution to be yellow. Remove any air bubbles and then inject into the muscle. You might feel a slight burning due to the acidity of some vitamins, but it should be brief. After injecting, apply gentle pressure with a clean cotton swab. Dispose of the needle safely in a sharps container. The frequency will be as prescribed, often once a week or as directed. Each time, vary the injection site (alternate legs, for instance) to prevent soreness or muscle irritation.
Always follow the instructions given by your healthcare team. If any questions arise, for instance, about needle size, or if you experience an injection site issue, consult your provider. With practice, many patients find IM self-injection to be straightforward. Ensure you keep the medication refrigerated as instructed and only draw it up when you’re ready to inject. By administering it correctly, you’ll get the full benefit of the vitamins.
What results or benefits should I expect to see, and how soon?
The benefits of Vitamin B-Complex Injection depend on your body’s needs. If you have a true deficiency of one or more of these vitamins, you may notice significant improvements as your levels are restored. Many patients may report an increase in energy and a decrease in fatigue after starting B-complex injections, usually within days to a couple of weeks of regular treatment. This is because B vitamins are crucial in converting food into usable energy (ATP), and correcting a deficiency allows your metabolism to run more efficiently.[3] For example, someone with borderline thiamine and B₆ deficiency might feel less “brain fog,” improved mood, and better stamina as those vitamins are replenished. If you had neuropathic symptoms (like numbness or tingling in hands/feet due to low B₆ or B₁), you might find those sensations gradually improving over a few weeks of therapy; nerves take time to heal, but adequate B vitamins remove the roadblock to nerve repair.
It’s important to set realistic expectations: this injection is not a stimulant or a “quick fix” like caffeine. If you are not deficient and are taking it as a supportive measure, you might not feel any dramatic change, and that’s okay. In such cases, the benefit is more behind-the-scenes, supporting your body’s biochemistry. You might notice subtle positives such as improved concentration, better appetite, or more restful sleep, but responses vary. Some athletes or individuals report feeling an “overall wellness boost.” On the other hand, if your levels were already sufficient, you may not perceive a difference in how you feel (since the body generally doesn’t utilize excess beyond its needs). The main goal is preventing problems (like anemia, neuropathy, etc.) that would occur if you were low in these vitamins.
If you are taking the injections for a specific medical reason, for instance, as part of recovery from surgery or illness, your doctor will monitor objective markers. They might do blood tests showing improvement (e.g., better red blood cell indices once B₆/B₁ levels normalize). In terms of how soon: some effects (like improved alertness) can be within a few days. Others, like correction of anemia or nerve symptoms, might take a few weeks of consistent therapy. It’s also possible to feel no obvious “sensation” at the time of injection, apart from maybe a warmth if given IV. That’s normal. The vitamins are doing their work quietly at the cellular level.
To gauge improvement, track specific issues you had before, for instance, frequency of mouth sores (which can occur with B deficiencies), or numbness in feet, or level of fatigue on a 10-point scale. Over a month, you and your provider can review those to see if the injection is helping. If you don’t notice any improvement and you were not deficient to begin with, it could mean your vitamin levels were adequate and the injection is simply maintaining that status. Always communicate with your provider; they may adjust dose or frequency or recheck vitamin levels as needed. In summary, expect gradual improvements rather than an immediate surge. The injection is repleting vital nutrients and supporting your metabolism; the benefits can be increased energy, better neurological function, and ensuring your body has what it needs for optimal health. Give it a few weeks and discuss any changes (or lack thereof) with your healthcare provider at follow-up.
Are there any side effects or risks I should watch out for?
For most people, side effects are minimal. The most common side effect is simply pain at the injection site; you might have some soreness, redness, or a small lump where the shot was given. This usually goes away in a day or two. Applying a warm compress and gently massaging the area can help disperse the vitamin solution and relieve discomfort. Another benign effect, as mentioned, is bright yellow urine for a day after the injection; that’s expected due to riboflavin and means your body is clearing out excess vitamins it doesn’t need.[4] You might notice your urine has a stronger B-vitamin odor as well (similar to when taking multivitamin pills), again, normal.
Some patients report a mild headache or a feeling of lightheadedness after an IM injection; this is not very common, but if it happens, sitting or lying down for a few minutes post-injection can help. Ensure you’re well-hydrated; sometimes the body’s metabolic response to the vitamins can very slightly transiently lower blood pressure or blood sugar, leading to dizziness, which fluids and rest can mitigate. If you’re prone to fainting with injections, let your provider know; you can take the shot lying down.
Allergic reactions are rare but possible. These could include symptoms such as itching, a rash/hives, swelling especially around the face or throat, or difficulty breathing. This would likely occur shortly after the injection (within minutes to an hour). If you ever experience these, seek emergency medical care; anaphylaxis to injectable thiamine, while extremely uncommon, has been reported.[1] For this reason, it might be advised to remain in the clinic for 10-15 minutes after the first injection to ensure you don’t react. Subsequent injections, if you’ve not reacted, are highly unlikely to suddenly cause an allergy, but maintain caution.
Because this formula contains niacinamide, a few people might experience a flushing reaction (warmth, redness of the skin) or slight itching, although niacinamide usually does not cause the intense skin flush that niacin (nicotinic acid) does.[9] If you do feel flush or itchy, it should be mild and short-lived. You can mention it to your doctor; they might slow down future injections or ensure you haven’t taken other vasodilators (like hot drinks or exercise immediately prior) that could amplify that effect.
There are some very rare side effects listed in medical literature (mostly when large doses are given): for example, one out of many thousands of patients might develop a disturbance in liver enzymes or a tingling in the fingers or toes. However, these are typically associated with long-term mega-doses far exceeding what’s in your weekly shot.[9] With the standard regimen, we do not expect any liver issues or nerve issues; your body will use what it needs and harmlessly eliminate the rest.
In summary, monitor the injection site (if pain increases or the area gets very red, hot, and swollen, inform your doctor as that could indicate injection-site infection, which is exceedingly rare with proper technique). Note any unusual symptoms throughout the day of the shot; if you were to get an allergic reaction, it would likely be soon after injection. For ongoing safety, keep your healthcare provider informed about how you’re feeling during the therapy. The vast majority of patients feel fine and benefit from the injection without any problems. Should any side effect worry you, don’t hesitate to reach out to your provider for advice.
Can I continue my multivitamin or other supplements while on this injection?
You should definitely inform your healthcare provider about all supplements and vitamins you are taking. In many cases, it’s fine to continue a multivitamin while on B-Complex injections, but it may not be necessary. This injection is already providing a high dose of several B vitamins, far above typical multivitamin doses. Taking an oral multivitamin on top likely won’t cause harm because excess B vitamins are water-soluble and your body will excrete what it doesn’t need.[4] However, consistently taking large amounts of vitamins from multiple sources could potentially increase the risk of side effects (for example, very high vitamin B₆ intake from multiple supplements over time can cause neuropathy, and high niacin from many sources could affect your liver). Your doctor might suggest pausing standalone B-complex pills or high-dose biotin etc., while you’re receiving these injections to avoid redundant therapy. Often, once injections start, patients discontinue separate oral B supplements, sticking to perhaps just a basic multivitamin or prenatal vitamin at most.
If you do continue a daily multivitamin, separate it from any interactions, for instance, don’t take other vitamins at the exact same time as certain medications like tetracycline antibiotics (all B vitamins can bind with tetracycline in the gut and reduce its absorption). But since your injection bypasses the gut, that particular interaction is not an issue for the injection itself; it would apply only to oral supplements.
In terms of other supplements: be cautious with energy drinks or so-called “vitamin shots” that might also contain high doses of B3 or B6. Combining those with your injection could push you into very high intake territory. While not acutely dangerous, it’s not advisable without medical supervision. On the flip side, certain supplements might complement your therapy, for example, if you’re also low in B₁₂ or folic acid (B₉), your doctor might have you take those additionally, since this particular injection doesn’t include B₁₂ or folate. Often, B₁₂ is given as a separate injection if needed.
Bottom line: coordinate all supplements with your healthcare provider. They may say “it’s okay to stay on your multivitamin, it’ll just ensure you’re getting everything else too,” or they may prefer you stop it during injection treatment to accurately assess what the injection alone is doing for you. There is no risk of dangerous overdose from typical multivitamins alongside the shot, but any more than that (like multiple high-dose supplements) should be avoided. And always avoid any unauthorized “megadose” vitamin regimens unless your provider approves; more is not always better, and your injection is already supplying a robust dose.
Does this injection include vitamin B₁₂? If not, do I need B₁₂ separately?
No, this particular formulation of Vitamin B-Complex Injection does not contain vitamin B₁₂ (cobalamin). It includes B₁, B₂, B₃, B₅, and B₆ as its active ingredients.[1] Many people colloquially think of “B complex” as all the B’s, but pharmacies actually prepare different combinations. Some B-Complex injections add B₁₂, but others (like the one you have) focus on the other five and omit B₁₂. Vitamin B₁₂ is often given as a standalone injection when needed, because B₁₂ has a large molecular size and specific storage dynamics; it’s usually administered intramuscularly or subcutaneously in doses like 1,000 mcg for deficiency, on its own. There are practical reasons too: B₁₂ can be unstable if mixed with certain other vitamins in solution, and dosing schedules for B₁₂ deficiency (pernicious anemia, for instance) may differ.
If your doctor suspects or knows that you also need B₁₂, they will likely prescribe it separately. For example, some patients get a B₁₂ shot (methylcobalamin, cyanocobalamin or hydroxocobalamin) once a month in addition to weekly B-Complex shots. B₁₂ is crucial for nerve health and blood cell formation, but not everyone getting B-Complex injections will need B₁₂; it depends on your levels. Commonly, individuals with malabsorption or anemia might actually receive a combination therapy: a B-Complex injection and a B₁₂ injection. In other cases, if your B₁₂ level is normal and you’re just low in the other B’s, your provider might intentionally choose a B-Complex without B₁₂ to avoid unnecessary injections.
It’s a good idea to clarify with your healthcare provider whether your B₁₂ status has been checked. If it hasn’t and you’re exhibiting symptoms like fatigue, numbness, or anemia, ask if a B₁₂ test is needed. If you are low in B₁₂, an appropriate supplementation will be added. Keep in mind that oral B₁₂ is not well absorbed in people who truly lack intrinsic factor or have certain GI issues, which is why B₁₂ is usually injected or given as a high-dose sublingual in those cases.
In summary: This injection covers a broad range of B vitamins but excludes B₁₂ by design. Ensure you’re not missing B₁₂ if you need it. Your doctor may either assure you that your B₁₂ level is fine (so no B₁₂ needed), or they will arrange B₁₂ shots in tandem if necessary. It’s important because B₁₂ deficiency can cause serious issues like pernicious anemia and nerve damage; so it should be addressed separately. Always follow your provider’s guidance on this. If you are getting both injections, they can even be given on the same day (different syringes, possibly different sites). But do not assume B₁₂ is in the mix unless explicitly stated. Check the label on your vial: it lists exactly what’s inside. Since it doesn’t list B₁₂ (often called cyanocobalamin on labels), that confirms you’d need a separate source for B₁₂. Make sure you’re covered on that front, either via diet, supplements, or injection, as appropriate for your situation.
Do I need to follow any special diet while using this injection?
Generally, no special diet is required specifically because of the B-Complex Injection; but supporting your health with a balanced diet is always a good idea. The injection is providing you with the necessary B vitamins regardless of your food intake, which is helpful especially if you have trouble eating a balanced diet (due to illness or other reasons). However, maintaining a nutritious diet can synergize with the treatment. For example, while the injection covers B₁, B₂, B₃, B₅, B₆, you still need other vitamins (like vitamin C, B₉ folate, B₁₂ if not supplemented separately, etc.) and minerals (iron, zinc, etc.) from food. So a well-rounded diet ensures you’re not deficient in those areas either.
You don’t need to load up on additional B-rich foods to “help” the injection; you’re already getting an ample supply through the shot. But including foods high in these vitamins (like whole grains, meats, eggs, dairy, leafy greens, nuts) as tolerated can help maintain levels once the course of injections is over. Essentially the injection may be a temporary measure to fix levels; long-term, a good diet will help sustain them. If your condition allows, try to eat regular meals with protein and complex carbohydrates to support your metabolism; B vitamins work to convert those nutrients into energy, so giving your body quality fuel (like lean meats, fish, legumes for protein; whole grains for carbs) can maximize the benefit.
One note:alcohol consumption can drastically deplete B vitamins (especially thiamine and folate). If you are being treated with B-Complex injections, it may be because of alcohol-related deficiency (common in chronic alcohol use). It would be wise to moderate or avoid alcohol during your treatment, or you could undermine the progress. Similarly, certain foods or medications that interfere with B-vitamin absorption aren’t a concern since absorption isn’t reliant on the gut here, but overall health habits matter.
No specific food will counteract the injection, so there are no “forbidden” foods due to the shot. But as a good practice, maintain hydration and adequate protein intake; vitamins act as catalysts, and proteins and calories provide the substrate for them to work on. There’s also no need to take extra oral vitamin supplements unless directed; the injection is potent.
In summary, follow a normal healthy diet. If you were on any dietary restrictions for other medical reasons, continue those as instructed by your doctor or dietitian. The injection doesn’t require you to fast or avoid anything. After the injection, you can eat and drink as usual. If anything, the improved B-vitamin status might increase your appetite or how your body processes foods efficiently. Keep communicating with your healthcare provider; sometimes they may recommend a nutrition plan tailored to your condition (for instance, high-protein diet if you have wounds to heal, etc., along with the vitamins). Think of the B-Complex Injection as one piece of the overall health puzzle; diet and lifestyle are the other pieces that complete the picture.
How long will I need to take these injections?
The duration of therapy with Vitamin B-Complex Injection depends on the reason it was prescribed. If you have a temporary deficiency or increased requirement (say, after a surgery or during recovery from an acute illness), you might only need a short course, perhaps a few weeks of injections, until your vitamin levels normalize or you can meet your needs by mouth again. For example, a patient with severe flu and poor intake might get weekly shots for a month and then stop once they’re eating well. In cases of documented vitamin deficiency, the regimen could be an initial intensive phase (like 2 mL IM three times a week for 2 weeks) followed by reevaluation. Once blood levels and symptoms improve, the doctor may discontinue the injections and advise maintaining levels with oral supplements or diet.
On the other hand, some conditions require long-term or even lifelong supplementation. If you have malabsorption syndrome (such as short bowel syndrome, certain bariatric surgery patients, chronic pancreatitis, or celiac disease that severely impairs nutrient uptake), you might need these injections indefinitely to prevent recurrent deficiencies. Patients on chronic total parenteral nutrition (TPN) often receive a formulation of vitamins similar to this on a continuous basis. Another example: individuals with chronic alcoholism often need prolonged thiamine/B-complex support; while the acute repletion might be IV/IM for a period, they may transition to high-dose oral vitamins thereafter.
Your doctor will typically monitor your response and perhaps repeat blood tests for vitamin levels (or relevant markers like homocysteine levels, complete blood count, etc.) after a certain number of injections. Based on those results and how you’re feeling, they’ll decide to continue or taper off. Some patients might move from, say, weekly injections to monthly injections as maintenance, then eventually to none if possible. Others might switch to an equivalent high-quality oral B-complex once their gut can absorb again.
So, there is no one-size-fits-all answer; it could be 1 month, 3 months, or longer-term. Always follow up as scheduled so your provider can make that decision with you. It’s important not to stop the injections prematurely on your own; if they were prescribed to correct a deficiency, stopping too soon could mean it comes right back. Conversely, if you’ve been on them a long time, check in to see if it’s still necessary at the same frequency. The regimen could possibly be adjusted down if your levels are consistently good.
Ensure you understand the plan at each stage: ask your doctor “How long do we anticipate I’ll need these?” at the outset, and at follow-ups ask “Are we going to recheck levels or try stopping soon?” This will give you a sense of the expected duration. In summary, use the injections for as long as they are providing a clear benefit and need. Your healthcare team’s goal will be to continue them until it’s safe to stop (if possible). Some patients view these shots as a short-term boost, others as a maintenance therapy. Both scenarios are valid depending on the underlying health context.
Administration Instructions
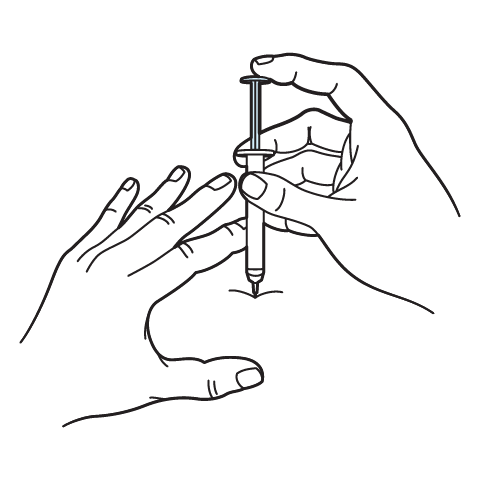
Intramuscular Injection Instructions
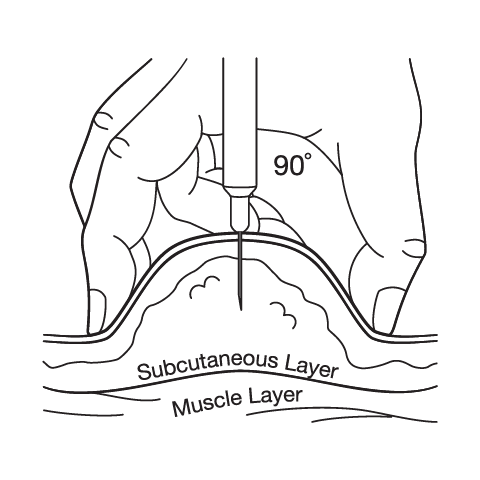
Subcutaneous Injection Instructions
Related medications
503A vs 503B
- 503A pharmacies compound products for specific patients whose prescriptions are sent by their healthcare provider.
- 503B outsourcing facilities compound products on a larger scale (bulk amounts) for healthcare providers to have on hand and administer to patients in their offices.
Frequently asked questions
Our team of experts has the answers you're looking for.
A clinical pharmacist cannot recommend a specific doctor. Because we are licensed in all 50 states*, we can accept prescriptions from many licensed prescribers if the prescription is written within their scope of practice and with a valid patient-practitioner relationship.
*Licensing is subject to change.
Each injectable IV product will have the osmolarity listed on the label located on the vial.

Given the vastness and uniqueness of individualized compounded formulations, it is impossible to list every potential compound we offer. To inquire if we currently carry or can compound your prescription, please fill out the form located on our Contact page or call us at (877) 562-8577.
We source all our medications and active pharmaceutical ingredients from FDA-registered suppliers and manufacturers.


 Pyridoxine HCl Injection
Pyridoxine HCl Injection Thiamine HCl Injection
Thiamine HCl Injection Folic Acid (Vitamin B9) Injection
Folic Acid (Vitamin B9) Injection Dexpanthenol (Vitamin B5) Injection
Dexpanthenol (Vitamin B5) Injection Cyanocobalamin (Vitamin B12) Injection
Cyanocobalamin (Vitamin B12) Injection Ascorbic Acid (Vitamin C) Injection
Ascorbic Acid (Vitamin C) Injection Magnesium Chloride Injection
Magnesium Chloride Injection Calcium Gluconate Injection
Calcium Gluconate Injection Methylcobalamin Injection (Vitamin B12)
Methylcobalamin Injection (Vitamin B12)